Autor: Carlos de la Torre Domingo.
Diplomado Universitario en Fisioterapia.
Profesor de Fisioterapia.
Universidad Alfonso X “El Sabio”. Madrid.
Titular en la Residencia de la Tercera edad “Bellas Vistas”.Madrid.
INDICE
1. Introducción.
2. Etiología.
3. Clínica:
-Acinesia.
-Rigidez.
-Temblor en Reposo.
4.Valoración del Paciente Parkinsoniano:
-Valoración del aparato Locomotor.
-Valoración de otros Sistemas.
5.Tratamiento Fisioterápico:
-Actividades Cinesiterápicas.
-Control de la Tendencia de la Postura en Flexión.
-Ejercicios para la autonomía Personal.
6. Consideraciones Personales.
7. Bibliografía.
1. Introducción
La Enfermedad de Parkinson es un síndrome extrapiramidal progresivo, que se debe a una afectación de los ganglios basales. Esta enfermedad fue descrita por el médico James Parkinson en 1817.La Enfermedad de Parkinson y el síndrome parkinsoniano comprenden un grupo de trastornos caracterizados por temblor y alteración del movimiento voluntario, postura y equilibrio.
El “ Síndrome Parkinsoniano” es el grupo de alteraciones en que se desarrollan los síntomas y signos característicos del parkinsonismo, pero en forma secundaria a otra enfermedad neurológica, como por ejemplo en parkinson de origen vascular o en la enfermedad de Alzheimer. Así, mientras que la Enfermedad de Parkinson es un trastorno degenerativo primario que se produce en la segunda mitad de la vida y sigue un curso progresivo, el síndrome parkinsoniano tiene una historia natural que depende de su causa.
Los síndromes extrapiramidales podemos encontrárnoslos de dos tipos;
a- Síndrome extrapiramidal de tipo acinésico – rígido: Esto se da en la enfermedad y síndrome de Parkinson.
b- Síndrome extrapiramidad de tipo hipercinético o hipotónico: Estos son por ejemplo; corea, atetosis, hemibalismo, distonias.
El sistema extrapiramidal tiene las siguientes funciones:
a- Control y ajuste de la secuencia de los movimientos automáticos., cuando se lesiona esta función se produce; Temblor y Distonía.
b- Regulación del tono muscular; cuando se altera esta función se produce, Rigidez y Acinesia o Bradicinesia.
c- Regulación de las reacciones posturales.
d- Armonización de la actividad motriz.
2. Etiología
Los síntomas y signos del parkinsonismo se originan en una alteración de la función en dos regiones de los ganglios basales, La sustancia negra y el cuerpo estriado ( Núcleo caudado y putamen). Estas masas nucleares centrales de materia gris contienen prácticamente toda la Dopamina del encéfalo humano. La dopamina es una sustancia química y una de las aminas neurotransmisoras que transportan el mensaje eléctrico desde una neurona a la próxima a través de la sinapsis.
La enfermedad de parkinson es responsable de la enorme mayoría de casos de parkinsonismo. La causa de la degeneración de la sustancia negra y del cuerpo estriado es desconocida, pero es un proceso progresivo y con una duración entre el comienzo y la muerte de entre 10 y 15 años; en los peores casos, la inmovilidad creciente lleva a complicaciones asociadas como son, Úlceras por presión, pérdida de peso y complicaciones respiratorias, que son la causa habitual de muerte.
3. Clínica
Esta enfermedad presenta una clínica característica que a continuación se detalla y posteriormente se explicará cada punto.
a- Acinesia: Falta de movimiento, o bien hipocinesia que es la disminución en la ejecución de los movimientos.
b- Rigidez: es el aumento de tono muscular no velocidad dependiente, así se diferencia de la espasticidad.
c- Temblor en reposo; Este punto es muy importante, el temblor como signo neurológico puede ser de dos tipos, temblor de intención como se da en el síndrome cerebeloso , o temblor en reposo, como se da en el individuo con parkinson.
d- El comienzo de esta enfermedad suele ser insidioso.
e- La evolución puede ser de dos tipos; lenta (inferior o igual a 10 años), o rápida (inferior a 4 años).
Acinesia: Efectos que produce la acinesia o hipocinesia en los pacientes enfermos con parkinson.
a- Dificultad para realizar dos patrones de movimiento simultáneos, como por ejemplo levantarse y saludar.
b- Retraso y lentitud en el inicio y ejecución de los movimientos voluntarios.
c- Pérdida de movimientos voluntarios y automatismos, por ejemplo pierden la secuencia normal de parpadeo en los ojos, pierden el balanceo de la cintura escapular y pélvica durante la marcha, esto último pone en compromiso el equilibrio del tronco durante las fases de marcha.
d- Amimia; Disminución de los gestos de la mímica facial. “Fascies en Máscara”.
e- Fatigabilidad a la ejecución de movimientos repetidos.
f- Disfagia.
g- Voz lenta, monótona y poco modulada.
h- Marcha lenta, pasos cortos, sin braceo, dificultad para los giros al caminar y también para los giros en el decúbito.
i- Alteraciones en la escritura, suelen tener una letra muy pequeña (micrografía) , esta alteración es por la disfunción en los movimientos de coordinación fina que implica la escritura.
j- Lentitud en la realización de las A.B.V.D.
Rigidez: Efectos que produce la rigidez en los pacientes enfermos de parkinson.
a- Se evidencia una Rigidez Cerea; esto es una rigidez continua, no tiene fenómeno en navaja, y si tiene el fenómeno de la “Rueda Dentada”, esto aparece porque a la rigidez se les une el temblor.
b- A consecuencia de la rigidez se les produce dolores musculares, torpeza motora, no tienen trastornos de la sensibilidad.
c- Biomecánicamente adquieren una postura hipercifótica en bipedestación, incluso en sedestación.
Temblor de reposo: Características del temblor en el Parkinson.
a- Suele ser rítmico.
b- Presenta una oscilación lenta; aproximadamente de 4 a 6 ciclos por segundo.
c- Afectación inicialmente unilateral a una de las manos.
d- Cede con la actividad.
e- Cede con el sueño.
f- Aumenta con la tensión emocional.
g- No suele temblar la región de la cabeza.
4. Valoración del paciente Parkinsoniano
La valoración podemos estructurarla de la siguiente forma:
Valoración del aparato locomotor:
Valoración Mecánica:
Balance articular
balance muscular.
Valoración Neurológica:
Postura
equilibrio
temblor.
Valoración Funcional:
ABVD
motricidad fina
marcha.
Otros sistemas:
Psíquico.
Otros Sistemas.
a- Postura: Suele tener una tendencia a la postura en flexión, hipercifótico en bipedestación y también persiste en sedestación.

b - Equilibrio: Las valoraciones del equilibrio hay que realizarlas en bipedestación, en sedestación y en apoyo monopodal, en estas valoraciones hay que explorar los equilibrios en los sentidos anterior, posterior y lateral.
c- Valoraciones funcionales: Valoraciones en la realización de tareas sencillas, valoración de la marcha, valoración de la motricidad fina, valoración del nivel de discapacidad. Asociaremos a estas valoraciones una valoración articular completa, para analizar posibles retracciones, y un balance muscular sobretodo para analizar el grado de rigidez de la postura, acortamientos tendinosos.
d- Valoración de otros aspectos como son; temblor, estado psíquico, alteraciones respiratorias.
5. Tratamiento de Fisioterapia
El objetivo de la fisioterapia en esta enfermedad sería ayudar al paciente a mantener su independencia tanto como fuera posible y aconsejar a los familiares y ayudantes como manejar a la persona afectada a medida que la actividad progresa y se establecen las incapacidades, los familiares tienen que adquirir unas características especiales pues como está descrito en la clínica algunos signos aumentan con la tensión emocional.
El tratamiento comenzará precozmente y durará toda la vida, con la programación de ejercicios domiciliarios y las revisiones médicas establecidas.
Estos pacientes han perdido el automatismo, así es importante conseguir movimientos amplios, repetidos, rítmicos y conjuntados.
El tratamiento podemos organizarlo de la siguiente forma:
1. Actividades Cinesiterápicas.
1.a- Para la prevención de retracciones y su tratamiento:
Intentamos prevenirlas mediante movilizaciones pasivas y activas asistidas, si ya tienes establecidas las retracciones, usaremos, termoterapia, cinesiterapia pasiva favoreciendo elongación de musculatura acortada, trabajo concéntrico de la musculatura antagonista a la acortada y uso de férulas progresivas.
2. Control de la tendencia de la postura en flexión.
Para conseguirlo haremos:
Ejercicios concéntricos de extensión de tronco.
Ejercicios concéntricos de ABD de caderas.
Ejercicios concéntricos de extensión de rodillas.
Ejercicios concéntricos y alternativos de flexión dorsal y plantar de tobillos.
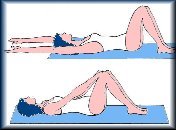
Tenemos que tener en cuenta que en estos pacientes se produce una ventralización del centro de gravedad, por esta razón aumentan los patrones flexores sobre los extensores, siguiendo este razonamiento es tan importante reducir esos patrones como inhibirlos por ello estos ejercicios son mucho más favorables realizarlos con el paciente en decúbito supino ya que esta posición por si sola inhibe los patrones flexores. Y por otro lado en esta posición ya no importa el desplazamiento del centro de gravedad que ellos padecen, normalmente en el decúbito se ve reducido el temblor.
3. Ejercicios para la autonomía personal:
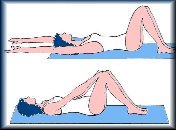
3.a- Ejercicios realizados sobre la cama o el suelo:
Son ejercicios realizados pasando de un decúbito a otro, acentuando al voltear la rotación inicial de cuello y ayudándose el paciente de sus miembros superiores para voltearse.
Movimientos de un miembro superior y uno inferior opuesto imitando la disociación escápulo pélvica que ha de suceder en la marcha.
Movilizaciones rítmicas, simétricas y simultaneas de 2 miembros superiores, de 1 miembro inferior y de los 2 miembros inferiores de forma simultanea.
Desde el suelo a la cama hacemos ejercicios de incorporación o elevación desde el decúbito supino, ayudándose de sus miembros superiores.
3.b- Ejercicios en sedestación:
Estos ejercicios los haremos una vez que el paciente controla los ejercicios citados en el apartado anterior.
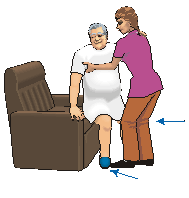
Ejercicios de sentarse y levantarse, controlando que haga flexión de tronco para desplazar el centro de gravedad y ayudándose de sus miembros superiores, en su defecto se le asistirá en el paso de sedestación a bipedestación.
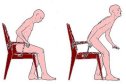
Ejercicios activos de flexión, extensión y rotación de cuello y tronco, estos ejercicios se los indicamos de forma rítmica, incluso enumeramos los movimientos para estimular la integración de los mismos.

Ejercicios de estimulación del equilibrio al empuje en sedestación, para que el paciente mantenga un buen equilibrio anterior, posterior y lateral en bipedestación previamente lo tiene que tener en sedestación.
3.c- Ejercicios en bipedestación:
Al igual que antes es conveniente realizar estos ejercicios una vez supere los anteriores.
Ejercicios de control postural frente al espejo, así trabajamos la simetría postural principalmente en el plano frontal, si hay posibilidad de espejos haremos lo mismo para que el paciente se visualice en plano sagital y corrija la postura.

Ejercicios de elevación desde el suelo o de descenso al suelo y si puede los hará ayudándose de los miembros superiores, a distintos ritmos y a distintas velocidades.
Ejercicios de equilibrio disminuyendo progresivamente la base de apoyo hasta llegar a hacerlo en apoyo monopodal.
Ejercicios de marcha estática con movimientos coordinados de balanceo de miembros superiores y miembros inferiores, simulando marcha hacia delante y hacia atrás, marcha salvando pequeños obstáculos.
Ejercicios de transferencias de peso y giros sobre su eje vertical.
3.d- Ejercicios de marcha o práctica de marcha:
Se harán a pasos muy largos, con mucha flexión y extensión de rodillas, en general son pasos muy exagerados.
Hay que evitar las posturas atascadas, cuando el paciente va a comenzar la actividad de empezar a andar se queda atascado y en ese momento le daremos un empuje o estímulo para que inicie el paso, también lo podemos evitar haciendo que siga unas marcas simétricas en el suelo, por ejemplo una huellas pintadas.

Practicar la marcha hacia atrás y de lado, salvando obstáculos.
6. Consideraciones Personales:
Como sucede en todas las patologías degenerativas, cuando nos encontramos frente a un paciente de estas características, tiene que prevalecer más en nosotros el entusiasmo por conseguir hacer de ellos personas funcionales, esta patología no tiene porque ir asociada a un deterioro cognitivo y esto provoca al paciente una problemática que nosotros hemos de minimizar, pues él o ella se da perfectamente cuenta de lo que su cuerpo está experimentando, tenemos que conseguir con las actividades médicas, fisioterápicas y de terapia ocupacional, hacer de su clínica algo positivo, interpretado como mejora de su calidad de vida a la cual todos tenemos derecho independientemente de nuestra situación clínica basal.
7. Bibliografía:
· R. González Mas; Rehabilitación Médica de Ancianos. Ed. Masson.D.L. B.33.606-1995.
· Alan Frazer, Perry Molinoff, Andrew Winokur; Bases Biológicas de la Función Normal y Patología del Cerebro. Ed. ESPAX. D.L: B. 29.840.1995.
· Rafael González Maldonado; El Extraño Caso del Doctor Parkinson. Ed. Grupo Editorial Universitario.D.L. G.R – 947-97.
· J.T. Meadows; Diagnóstico Diferencial en Fisioterapia. Ed. McGraw –Hill. D.L. M 37.859-2000.
· Downie; Neurología Para Fisioterapeutas. Ed. Panamericana. ISBN 950-06-0365-9.
· R. Alberca, J,J, Ochoa; Neurogeriatría. Ed. J.Uriach & Cía. S.A. ISBN 84-604-2757-9.
